Co-Occurring Disorders in Drug & Alcohol Rehab
Fighting an addiction may be the hardest thing you ever do - unless, of course, you have a co-occurring disorder. As the name implies, a co-occurring disorder refers to the simultaneous existence of two conditions. Most addiction experts use the term to apply to two mental health issues - such as addiction and anorexia - but some also refer to simultaneously occurring physical and mental health problems as co-occurring disorders.
No matter what disorder or group of health problems you face, you are not alone. A surprisingly high number of addicts are forced to wrestle with co-occurring disorders. Indeed, it's often the co-occurring disorder that spurs an addict to get treatment in the first place. To recover, though, you first need to understand the nature of each of your diagnoses, as well as how your conditions interact with one another.

Dual Diagnosis: Facing Addiction and Mental Illness
A dual diagnosis occurs when you experience a mental illness and an addiction at the same time. About half of all addicts also have a mental illness, causing some addiction experts to suggest that similar brain pathways may be implicated in both substance abuse and mental illness. Research is still in its infancy in this area, so we don't really know why so many people with mental health issues develop addictions, but experts have suggested several possible explanations.
First, mental illness makes life much more difficult than it otherwise would be. From coping with the search for the right treatment to dealing with loved ones who don't accept that mental illnesses are real illnesses, the everyday reality of life with mental illness can be extraordinarily demoralizing. Some people with mental illness turn to drugs to cope with the pain.
Second, mental illness and addiction both have the capacity to radically upend your life. Either can destroy your relationships, undermine your career, change your behavior, and sap your motivation. And thus one can lead to the other. For instance, if your depression harms your marriage, you might turn to alcohol to cope. Or if heroin harms your relationship with your child, you may end up with depression.
Finally, treatments for mental illness may cause addiction in some cases. Anti-anxiety medication such as Klonopin, for example, are highly addictive. Likewise, your doctor may prescribe sleeping pills, or recommend drugs to help you deal with the chronic pain that sometimes co-occurs with mental illness. While anyone can become addicted to these drugs, people with mental illness are especially vulnerable, creating a cruel irony in which the treatment for your disease leads to another. The good news, though, is that it's often possible to find less-addictive treatment options, and some mental illnesses can be well-managed with therapy and lifestyle changes alone.

Do I Have a Mental Illness?
So how do you know if you have a mental illness in the first place? We all feel emotionally out of control from time to time, and a few instances of "abnormal" behavior does not mean you are mentally ill. There are hundreds of mental illnesses, too, so if you have a rare condition, it may be hard for you to even locate information about your symptoms. Mental illnesses are characterized by pervasive patterns of unhealthy or damaging behavior that is not better explained by something else. Mental illness also negatively affects your life. For example, a woman who has just lost her spouse might cry all the time, but this is a normal reaction to grief, not necessarily a sign of depression. Similarly, a woman with unusual interests in plants might seem "strange" or "crazy," but if the interest does not interfere in her ability to function, she is not mentally ill. Some other differences between mental illness and the normal continuum of weird human behavior include:
- You can't think mental illness away. You can give up procrastinating with enough dedication, but dedication won't cure depression.
- Mental illness persists across circumstances. If you feel depressed in an abusive or bad marriage, you don't have depression if you feel better when you get out of the marriage.
- Mental illness continues to exist no matter who you spend your time with, though some people with mental health issues are very good at hiding their symptoms from people outside of their household.
- Mental illness isn't about being weird or eccentric; mental illness undermines your ability to live a productive or happy life, harms your relationships with others, or both.

Common Mental Illnesses
Knowing the most common mental health conditions, as well as their symptoms, can help you get a diagnosis faster, particularly if you struggle to discern how much of your behavior is due to addiction and how much is due to mental illness. And once you know that your feelings are part of a larger illness and not due to a personal failing, you may feel better equipped to fight both your mental illness and your addiction.
This isn't an exhaustive list, so if you're worried that you might be mentally ill, consult your physician. And remember, some people experience unusual presentations of an illness. For example, many men with depression feel angry, not hopeless or sad.
Anxiety disorders, as a group, are the most common type of mental illness in the world. This group of conditions includes several different disorders, each with its own distinct set of symptoms
Generalized anxiety disorder is characterized by chronic, free-floating anxiety. You may have difficulty sleeping, experience nightmares, wake up with your heart racing, or feel constantly fearful for no apparent reason. Many people with GAD experience their anxiety as physical sensations, so it's common for GAD sufferers to report unexplained ailments, aches, and pains.
Panic disorder causes panic attacks - moments of overwhelming panic during which you may feel like you are going to die. These attacks can be debilitating, and some people with panic disorder are so afraid of having a panic attack in public that they develop a second disorder, agoraphobia. Agoraphobia is the chronic fear of going out in public, and - in extreme cases - can cause its sufferers to become completely shut-in recluses.
Post-traumatic stress disorder is one of only a handful of mental illnesses that has a clear cause. To qualify for a diagnosis of PTSD, you must experience a serious trauma, such as rape, a natural disaster, military combat, or a serious car accident. People with PTSD experience anxiety, depression, anger, and recurring intrusive memories known as flashbacks. They may also experience nightmares,
Obsessive disorder is characterized by anxious obsessive thoughts. For instance, a pregnant woman might be preoccupied by fears of a miscarriage, or a man with a flying phobia might be convinced his plane is about to crash. To alleviate these chronic obsessive thoughts, people with OCD engage in compulsive behaviors. The compulsive behavior varies significantly from person to person, but often includes counting, tapping, or cleanliness-related tasks, such as cleaning or washing the hands.
A person with OCD might engage in these rituals hundreds of times each day. For example, a person concerned about premature death might begin tapping all objects in the house eight times every day, till that activity eventually takes up all or most of her time.
Mood disorders are disorders that lower your mood. The best-known is depression, which causes pervasive feelings of sadness, shame, worthlessness, and hopelessness. Many people with depression also experience anger, relationship problems, sleep disturbances, changes in appetite, and minor aches and pains.
A related disorder, dysthymia, yields less severe symptoms than depression, but lasts longer - often for years. Bipolar disorder - sometimes known as manic depression - is a cyclical disorder. People with this condition go through cycles of depression, followed by cycles of manic emotions and activity.
Personality disorders fundamentally alter the way you view yourself and interact with the world. Because they affect everything about your personality, though, they can be hard to diagnose. A few personality disorders include:
- Borderline personality disorder - characterized by chronic instability in relationships, terror of being abandoned, and alternating between idealizing and devaluing loved ones.
- Narcissistic personality disorder - leads to relationship difficulties, and can give rise to cruel behavior. People with narcissistic personality disorder are highly self-involved, and often do not care about the suffering of others.
- Histrionic personality disorder - characterized by chronically out of control emotions and attention-seeking behavior.
- Antisocial personality disorder - sometimes referred to as sociopathy, this personality disorder results from little or no empathy.
Eating disorders are among the most dangerous mental health conditions, ultimately killing about 10% of their victims. Many people with eating disorders turn to drugs and alcohol to attempt to increase weight loss or to numb the pain of body hatred. The three most common eating disorders are:
- Anorexia nervosa, which causes its sufferers to obsessively attempt to lose weight, usually through a combination of starvation dieting and compulsive exercise.
- Bulimia nervosa, which results in binge eating sessions followed by attempts to purge the food, usually by vomiting, but sometimes through the use of laxatives or enemas.
- Binge eating disorder, which causes sufferers to consume large quantities of food in short periods of time. Binge eating disorder may play a major role in the development of obesity.
Learning disorders affect their victims' ability to learn in the way most other people do. Sometimes called developmental disorders or developmental delays, learning disorders frequently accompany other mental health conditions. Stimulant drugs can effectively treat some learning disorders, but the addictive potential of these drugs predisposes users to developing a dependence. Some common learning disorders include:
- Attention deficit hyperactivity disorder (ADHD) - a disorder that results in hyperactive behavior, difficulty concentrating, problems with organization, and chronic restlessness.
- Dyslexia - causes difficulties with reading, writing, and occasionally, speech.
- Autism-spectrum disorders - these disorders compromise empathy, communication skills, and intellectual development. They can also cause sensory sensitivity, aggression, and a host of other behavioral abnormalities.
If you have a mental health condition, you need and deserve treatment for both your addiction and your mental health problem. As many as 60% of people with mental illness never seek treatment, even though mental illness is a leading cause of disability worldwide. Mental health issues are not your fault; they're no different from physical health issues, and with the right treatment, you can and will feel better.

Cross-Addictions: When You Struggle With Multiple Addictions
A cross-addiction occurs when you replace one addiction with another. It's common for addicts, especially in the early days of the recovery journey, to replace one substance with a similar substance. An alcoholic might replace alcohol with another depressant, such as heroin. A person addicted to shopping might get wrapped up in another compulsive behavior, such as gambling. You're most vulnerable to cross-addictions in the early stages of recovery. However, addiction is a disease that fundamentally alters the way you interact with the world. Thus a history of addiction means you will always be more vulnerable to a subsequent addiction.
Some addiction specialists also use the term cross-addiction to refer to two co-occurring addictions. These sorts of addictions are very common, with between 25% and 50% of addicts addicted to two or more substances. Alcohol and prescription drugs are the most common source of this type of cross-addiction, though it's possible to become simultaneously addicted to any two addictive substances. Northpoint Recovery provides quality alcohol treatment in Idaho or drug rehab for those facing a dual-diagnosis.

Substance Abuse
Most people with a cross-addiction become addicted to another drug. As with "typical" addiction, cross-addictions come with a hefty dose of denial. You may not realize you're addicted to a second substance, particularly if you've already kicked the first substance to which you were addicted. In this scenario, you may even feel elated, like you've found a substance that can help take the edge off of withdrawal without getting addicted.
Thus, just as you did with your first addiction, you'll need to take a long hard look at your behavior regarding your second addiction. Addiction's hallmark is continuing to use substances in spite of negative life consequences. Addiction also usually comes with physical or psychological dependence. If you're not sure whether you have a cross-addiction, here are some clues you might:
- You continually increase the dose of your drug of choice to get the same effects you once got with a much lower dose.
- You are drunk or high most of the time, or during every free moment you have.
- You go to work under the influence.
- You drive under the influence.
- You worry you won't be able to feel normal without drugs or alcohol.
- You experience anxiety, depression, or intense mood swings when you try to stop.
- Your day is structured around your next fix. For example, you might use your lunch break to get high or drink.
- You lie to yourself, or to people you love, about your drug or alcohol use.
- You break the law - by driving drunk, stealing, or doctor-shopping - to use drugs or alcohol.
- You have a family history of addiction.
- You've previously had an addiction.
- People you love have expressed concerns about your substance use.
- You've experienced financial difficulties because of drugs or alcohol.
- You have an untreated mental illness.
- You spend a significant portion of your time with addicts.
Co-occurring addictions, like normal addictions, only get worse with time. It doesn't matter if you've already treated the first addiction or you think you can use the skills you learned in rehab to treat the new addiction. Every addiction you have must be treated, and delaying treatment only delays your recovery, thereby allowing your addiction time to get worse and a chance to ruin the lives of people you love the most.
It doesn't matter if the drug you're addicted to is a legal one, such as medical marijuana, prescription medications, or alcohol. Legal drugs actually cause more deaths and more addictions than illegal once, due at least in part to the fact that people who are addicted to legal drugs frequently spend more time in denial.

Compulsive Behavior
Virtually everyone knows that drugs and alcohol are potentially addictive; many of us can remember learning this fact in preschool, when we attended drug prevention programs. It may come as a surprise, though, to learn that behaviors can be every bit as addictive as drugs, yet many people struggling with behavioral addictions never get the help they need.
When you participate in pleasurable and rewarding behaviors, such as shopping, gambling, or having sex, your brain releases dopamine. In some people - especially those who have a previous history of addiction and those who have an intensely stressful life - this sensation can become addictive. The addict believes the behavior is causing the pleasure, when it's really the dopamine. Consequently, the addict continues with the compulsive behavior, even when it wreaks havoc on his or her life.
Almost any pleasurable behavior can become addictive, but some behavioral addictions are more common than others. Some common behavioral addictions include:
- Shopping addiction -- This addiction commonly causes people to increase consumer spending, but any kind of buying can become addictive. A person with a shopping addiction might compulsively buy and hoard groceries, spend money on clothing she never even wears, or obsessively buy home decorations. Though more common among women than men, both men and women can suffer from shopping addiction.
- Gambling addiction - Compulsive gambling is one of the most common addictions, outpacing even alcohol addiction. About 16% of the population has struggled with gambling addiction at some point, and addiction to gambling often gives rise to other addictions, since gamblers often rely on drugs and alcohol to steel their nerves.
- Sexual addiction - Sexual addiction was only recently added to the DSM, the Bible of mental health disorders, so there's still some debate about how it is categorized. Liking sex, having a lot of sex, or engaging in sexual behavior most people disapprove of - such as BDSM or polyamory - is not a sign of sexual addiction. Instead, sexual addiction is characterized by compulsive sexual behavior that offers little gratification and that you feel like you "need." Some sex addicts reach a point where they no longer enjoy sexual interactions. Many lie or pay prostitutes to get sex.

What About Physical Health Problems?
Historically, the medical literature has treated mental and physical health as two distinct things. But there's not a line of demarcation between mental and physical health. One can cause the other, and people vulnerable to mental health issues are also vulnerable to physical health problems. Skeptical about the connection? A number of the ways mental and physical health intersect include:
- Mental health issues sometimes cause physical health problems. For example, anorexia can cause organ failure, life-threatening weight loss, and seizures.
- Some mental illnesses come with physical symptoms. People with depression often have unexplained aches and pains, while generalized anxiety disorder can cause heart palpitations and chest tension.
- In some cases, treatments for mental health conditions can cause physical symptoms.
- Addiction almost always causes physical health problems, and the symptoms of withdrawal often include physical symptoms
Thus many addiction specialists now include health problems under the broad umbrella of co-occurring disorders. Whether you consider your health condition a co-occurring disorder or not, though, you need to know that health problems can complicate addiction treatment, so it's important to address all of your health problems with your doctor.

How Co-Occurring Disorders Change Things
Denial is a classic symptom of addiction, and denial won't go away just because you have a co-occurring disorder. In fact, in most people, denial is even stronger when there's a co-occurring disorder, so if you think you might need help treating multiple conditions, don't hesitate to talk to your doctor. If you only treat one condition, it's possible that neither condition will improve. And in some cases, treatment for one condition could actually exacerbate symptoms of another condition.
So how does having a co-occurring disorder change the landscape of treatment? Co-occurring disorders affect treatment in many ways:
- Some medications are potentially addictive. If you seek treatment for an anxiety disorder, for example, you may be prescribed a potentially addictive drug.
- The side effects of treatment for one condition can exacerbate symptoms of another. For example, some depression drugs decrease sexual function. For a person with a sex addiction, this could lead to even more compulsive sexual behavior, since the decreased functioning makes it more difficult to get a "rush" from sex.
- An untreated mental or physical health condition can make sobriety extremely challenging, if not outright impossible. Withdrawal often causes depression and anxiety, so if you already have these conditions and are not treating them, withdrawal may be too much for you to tolerate.
- Two simultaneously occurring addictions can affect your health in dramatically different ways from a single addiction. For instance, mixing alcohol with stimulant drugs can be fatal, so it's critically important to get prompt treatment and excellent medical care.
If you have a co-occurring disorder, you need to treat both conditions at the same time. In most cases, this will mean attending inpatient rehab, but in all cases it means - at minimum - working under the guidance and supervision of a mental health counselor and a medical doctor.
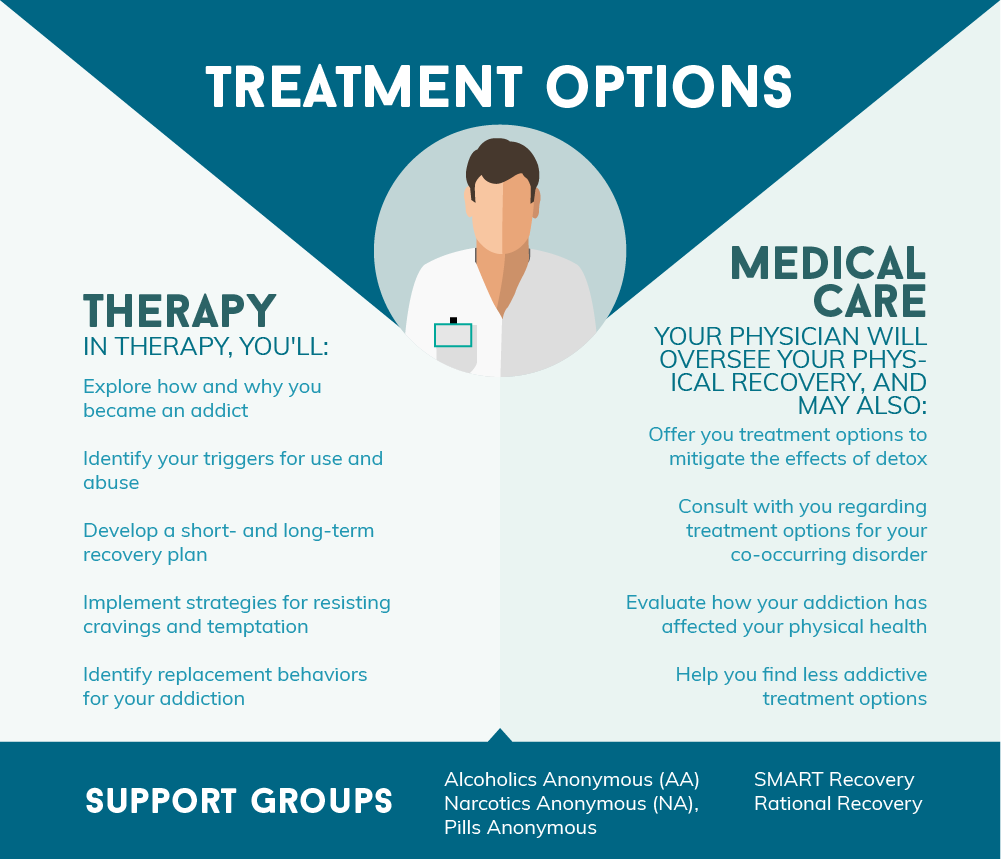
Treatment Options
If you suffer from a co-occurring disorder, rehab is the gold standard in treatment. Rehab offers comprehensive care designed to treat each of your symptoms, and ensures that your treatment is overseen by a skilled treatment team. In rehab, you'll gain access to the following services. You can also opt to independently pursue these treatment options when you complete rehab, or as you are waiting for a slot in the rehab center of your choice.
Every addict has a story, and no one voluntarily decides to suffer through the misery of addiction. A history of trauma or abuse, depression, relationship problems, and a host of other challenges can cause you to turn to addiction, especially if you suffer from a co-occurring disorder. In therapy, you'll:
- Explore how and why you became an addict, then work to identify why this specific drug is the one you use. For instance, if you rely on stimulants, your therapist will work with you to understand why the amplified feelings stimulants offer are appealing to you.
- Identify your triggers for use and abuse. For example, you might be more vulnerable to cravings when you're stressed.
- Develop a short- and long-term recovery plan.
- Implement strategies for resisting cravings and temptation.
- Identify replacement behaviors for your addiction. You might, for example, stop drinking alcohol and begin running.
Your relationship with your therapist is the single most important predictor of recovery, so choose a therapist with whom you feel comfortable and by whom you feel understood. If the therapist you get in rehab is not to your liking, ask for a different provider.
Medical care plays a key role in the recovery from both addiction and co-occurring disorders. Your physician will be charged with overseeing your physical recovery, and may also:
- Offer you treatment options to mitigate the effects of detox. In some cases, your doctor may be able to prescribe medications that reduce the severity of cravings or that decrease the unpleasant effects of withdrawal.
- Consult with you regarding treatment options for your co-occurring disorder. A doctor is the only person who can prescribe mental illness medications.
- Evaluate how your addiction has affected your physical health, and consult with you about how to best reduce the long-term effects of your addiction.
- Help you find less addictive treatment options. Many treatments for mental illness are potentially addictive, but a good doctor can help you determine which treatment is safest for you.
Support groups - notably those based on the 12-step model, such as Alcoholics Anonymous (AA), Narcotics Anonymous (NA), and pills anonymous - are among the most popular recovery programs. In fact, many people are able to get clean using these programs alone, but these programs will not treat a co-occurring disorder. By working the 12 steps, you'll make amends to those whom you've hurt, gain a deeper understanding of your addiction, and commit to a lifetime of sobriety.
These programs are peer-based, which means there is no expert oversight, but research suggests that peer support can play a key role in addiction recovery. 12-step programs are free, and meetings occur throughout the country at virtually every time of the day. If you need additional help outside of meetings, you also have the option to select a sponsor.
Though 12-step programs can be helpful, they are loosely spiritual, and some groups are explicitly religious. If you prefer a secular option, try SMART Recovery or Rational Recovery. Some rehab centers also offer group therapy, therapist-overseen support groups, and other alternatives to 12-step programs.
Many rehab facilities offer enrichment activities such as art therapy or yoga. These programs won't "cure" you on your own, but they can distract you from your cravings, help you master new skills, and offer you a healthier "addiction." If you've already left rehab or want to try going it alone, be sure to keep yourself busy. Busy people experience fewer cravings, and indulging your cravings is much more challenging when you're participating in an activity you enjoy.
To some extent, addiction is a lifestyle disease, since an unhealthy environment can make it much more challenging to get sober. While lifestyle remedies, in and of themselves, won't cure your addiction, they can make the recovery process more manageable. Try some of the following:
- Try to get at least 150 minutes of aerobic exercise per week.
- Eat a healthy, balanced diet rich in lean proteins, fruits, vegetables, and whole grains.
- Maintain a regular daily schedule.
- Commit to getting at least eight hours of sleep each night. Go to bed at the same time each evening, and try to get up around the same time each day.
- Remember that recovery requires time, so consider taking some time for yourself. Take a few days off of work, or ask your spouse to help with your kids. Addiction is a disease, and just as you might need some extra time and space to recover from surgery, you'll also need some time before you're fully recovered from an addiction or the withdrawal process.
- Tell loved ones about your decision to quit.
- Avoid other addicts, who may tempt you to use.
- Avoid places and situations that you associate with abuse of drugs and alcohol.
- Work to understand cravings. These discrete moments usually last about 10 minutes, so if you can ride it out, you'll quickly feel better.
- Nurture a safe and supportive home life. An abusive relationship, a dangerous neighborhood, and a stressful family life can all make it much harder to get clean.
- Treat your newfound sobriety as the beginning of a new life. By seeing sobriety as a holistic change to your entire life, you're much more likely to embrace recovery, and much less likely to see sobriety as giving something you love up.
- Take time to "mourn." Losing an addiction can feel a lot like losing a friend, so don't be ashamed if you need to cry a bit, take some time to miss your addiction, or work to accept that you'll never be able to use drugs or alcohol again.

The Road to Recovery
There's no escaping one central truth: the road to recovery is a long one, and it's usually even longer for people with co-occurring disorders. By viewing recovery as a journey - rather than a one-time decision - you can better equip yourself for this challenge. Remember, it is ultimately up to you whether you stay sober, and if you avoid drugs and alcohol, you will remain sober - no matter how challenging that sobriety is.
Addiction is a disease, and like other diseases, it comes with a high relapse rate. About half of all addicts eventually relapse, so any good recovery program should also include relapse prevention strategies.
The good news is that, even if you do relapse, the battle isn't over. Because relapse is so common, many addiction experts argue that relapsing is actually a part of the recovery process. Thus every time you relapse, you learn something new about your addiction, thereby increasing your chances of getting sober next time.
So how long can you expect to experience cravings? The short answer is that it depends. Your age, health, how long you've used drugs, and many other factors will affect the length and severity of the withdrawal process, but withdrawal usually only takes about a week or two. After that, things get much better. You may still have recurring cravings, but life no longer will feel like one big craving.
Most addicts have "triggers" - specific situations or experiences that previously triggered them to abuse drugs or alcohol. Facing down each of your triggers is key to recovery, since once you ignore a trigger, it will be much less likely to affect you in the future. As you systematically face each trigger, your cravings will get less serious and less frequent. This is a slow and steady process that, for many addicts, takes about a year. However, at the 3-month mark, many addicts are able to go days without thinking of drugs or alcohol, so don't be discouraged by this relatively long recovery timetable.
Your cravings will disappear, and you really can have a good life free of drugs and alcohol. Believing otherwise is merely th product of addiction. You may be feeling overwhelmed right now, but know that getting help is the first step on your recovery journey. You don't have to fight this battle alone, and millions of people just like you have successfully kicked drugs and alcohol for good.
Talk to a Rehab Specialist
Our admissions coordinators are here to help you get started with treatment the right way. They'll verify your health insurance, help set up travel arrangements, and make sure your transition into treatment is smooth and hassle-free.
Contact Us

















