How does binge-drinking lead to binge-eating?
It’s a well-known phenomenon—you go out drinking, and at the end of the night, you are so hungry, you end up gorging on cheap, greasy, readily-available fast food. LOTS of it. At first glance, that feeling of extreme hunger doesn’t seem to make much sense. Alcohol is the second-most calorie-dense foodstuff, after pure fat. Yet, rather than filling you up, drinking alcohol makes you even hungrier. Let’s take a look at what science has to say about how excessive drinking causes excessive eating.
Alcohol “evoked voracious feeding within minutes”
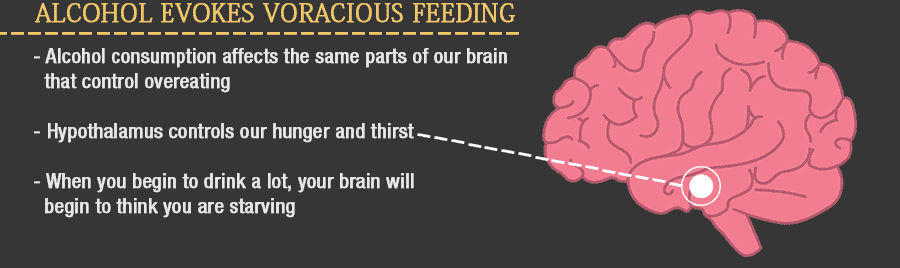 According to new research from the University College London and the Francis Crick Institute, the answer is in our brains. Alcohol consumption affects the same parts of the brain that control overeating. The region of the brain that controls hunger and thirst is the hypothalamus. Drinking directly affects specific structures – AgRp neurons – within the hypothalamus in the same way that extreme hunger does. In other words, when you drink heavily, your brain is “tricked” into thinking that you are starving. To explore that cause-and-effect in more detail, researchers gave laboratory mice an amount of alcohol that was roughly equivalent to a typical weekend bender. As expected, this causes those mice to eat more than another group that was not given alcohol. But significantly, when brain slices from dissected mice were dipped in alcohol, those neurons that were still living were activated—increased calcium production and a surge in electrical activity. To test those results, researchers again fed live mice alcohol, but this time, they blocked the AgRp neurons. The mice’s appetites did not increase.
According to new research from the University College London and the Francis Crick Institute, the answer is in our brains. Alcohol consumption affects the same parts of the brain that control overeating. The region of the brain that controls hunger and thirst is the hypothalamus. Drinking directly affects specific structures – AgRp neurons – within the hypothalamus in the same way that extreme hunger does. In other words, when you drink heavily, your brain is “tricked” into thinking that you are starving. To explore that cause-and-effect in more detail, researchers gave laboratory mice an amount of alcohol that was roughly equivalent to a typical weekend bender. As expected, this causes those mice to eat more than another group that was not given alcohol. But significantly, when brain slices from dissected mice were dipped in alcohol, those neurons that were still living were activated—increased calcium production and a surge in electrical activity. To test those results, researchers again fed live mice alcohol, but this time, they blocked the AgRp neurons. The mice’s appetites did not increase.
Drinking Increases the Appetite via the “Apéritif Effect”
 A pre-meal drink is known as an aperitif, from the Latin aperire — “to open”, because it was believed that alcohol “opened” the appetite. Even though the term is over 100 years old, it is startlingly accurate. Contemporary research suggests that even moderate consumption of alcohol can trigger an increase in both appetite and food intake. Using MRI technology, researchers at the Indiana University School of Medicine came to the following conclusions:
A pre-meal drink is known as an aperitif, from the Latin aperire — “to open”, because it was believed that alcohol “opened” the appetite. Even though the term is over 100 years old, it is startlingly accurate. Contemporary research suggests that even moderate consumption of alcohol can trigger an increase in both appetite and food intake. Using MRI technology, researchers at the Indiana University School of Medicine came to the following conclusions:
- Alcohol intoxication triggers the appetite and promotes binge-eating by increasing activity levels in the areas of the brain that control reward and regulate eating behaviors – the hypothalamus, the ventral frontal cortex, and the ventral striatum.
- Drinking significantly increases a person’s response to the smell of food.
- The entire test group as a whole ate more after they were given alcohol.
- However, a significant portion of the group ate considerably more — over 15% more.
In another study, it was determined that having 3 large glasses of wine can result in a person eating an extra 6300 calories over the next 24 hours!
Alcohol Changes the TYPES of Foods You Crave
 Another way that alcohol consumption contributes to overeating and to unhealthy weight gain is by changing the type of food that you want. In 2015, teams of researchers at the Netherlands Organization for Applied Scientific Research and the Division of Human Nutrition concluded that moderate alcohol intake had several effects on the amount and types of foods both craved and eaten. Consuming the equivalent of just one-and-a-half “standard” drinks resulted in increased:
Another way that alcohol consumption contributes to overeating and to unhealthy weight gain is by changing the type of food that you want. In 2015, teams of researchers at the Netherlands Organization for Applied Scientific Research and the Division of Human Nutrition concluded that moderate alcohol intake had several effects on the amount and types of foods both craved and eaten. Consuming the equivalent of just one-and-a-half “standard” drinks resulted in increased:
- Cravings for salty foods
- Enjoyment of salty and/or fatty foods
- Overall food consumption by 11%
- Consumption of salty and/or fatty foods by 24%!
Drinking Behaviors Influence Eating Behaviors
 Drinking keeps you from feeling full, causing you to eat well past the point of satisfaction. A 1997 study conducted by Laval University compared two groups of test subjects.
Drinking keeps you from feeling full, causing you to eat well past the point of satisfaction. A 1997 study conducted by Laval University compared two groups of test subjects.
- In the first group, men were given a high-fat appetizer, accompanied by an alcoholic drink.
- In the second group, men were given a low-fat appetizer, with a non-alcoholic drink.
Each selection contained the same number of calories, and there were no differences in hunger or fullness, as self-reported by the test subjects of both groups. Yet, the men in the first group—the high-fat/alcohol group– ate significantly more of the following entrée than those who were not served alcohol. Furthermore, the first group ate more than the low-fat/no-alcohol subjects did at their subsequent evening meal. In 2001, a Scottish study had test subjects visit their lab on three separate occasions. Each time, the volunteers were given either a non-alcoholic longer or a non-alcoholic beer that have been spiked with alcohol. Afterwards, the men were treated to a full buffet lunch. The results showed that whenever the subjects were given alcohol, they ate considerably more at the buffet. On average, they consumed 30% more calories. Yet another study, conducted in 2008, compared two groups of drinkers.
- Light drinkers – individuals who drank 1 or 2 times per month, consuming 2 or 3 drinks per occasion.
- Heavy drinkers – individuals who drank 1 to 3 times per week, consuming 4 or 5 drinks per occasion. In other words, binge drinkers.
The heavier drinkers had a greater tendency towards:
- Increased appetite
- Overeating after drinking
- Higher body mass index
The Missing Link between Alcohol and Appetite?
 In 2004, researchers at Princeton University suggested a source behind the related cravings for fatty and alcohol. Galanin, a neuropeptide found within the brain, may be the biochemical “missing link”. Among other functions, galanin plays a role in feeding, cognition, and mood recognition. Of special relevance, galanin has been linked to eating disorders. Galanin has a reciprocal relationship with alcohol. Drinking causes the body to produce more galanin, and excess galanin results in a stronger craving for alcohol. It is a self-perpetuating cycle of behavior. But here’s the key, as University of North Carolina research scientist William Gruchow explains, “Galanin increases appetite or fats, and consumption of fat causes more galanin to be produced.” Alcohol, fat, and the brain chemical galanin, all inextricably intertwined.
In 2004, researchers at Princeton University suggested a source behind the related cravings for fatty and alcohol. Galanin, a neuropeptide found within the brain, may be the biochemical “missing link”. Among other functions, galanin plays a role in feeding, cognition, and mood recognition. Of special relevance, galanin has been linked to eating disorders. Galanin has a reciprocal relationship with alcohol. Drinking causes the body to produce more galanin, and excess galanin results in a stronger craving for alcohol. It is a self-perpetuating cycle of behavior. But here’s the key, as University of North Carolina research scientist William Gruchow explains, “Galanin increases appetite or fats, and consumption of fat causes more galanin to be produced.” Alcohol, fat, and the brain chemical galanin, all inextricably intertwined.
Are Alcohol Use Disorder and Eating Disorders Related?
 Binge-eating is overeating past the point of fullness or satisfaction. And, as explained above, alcohol use can influence eating habits. But there is another line that can be crossed. Does your binging—
Binge-eating is overeating past the point of fullness or satisfaction. And, as explained above, alcohol use can influence eating habits. But there is another line that can be crossed. Does your binging—
- Happen in secret?
- Occur when you are stressed, angry, lonely, or afraid?
- Interfere with your social, family, or work life?
- Frequently go beyond your control?
- Bring your feelings of shame or guilt afterwards?
If you answered “yes” to any of these questions, you may have a diagnosable eating disorder. Binge-eating is the most-common eating disorder in the United States. Eating disorders are real illnesses that require specialized professional care if you are to restore healthy control, balance, and manageability to your life. In this way, eating disorders and addiction are very similar. In fact, the relationship between these seemingly-unrelated conditions is much closer than you think:
- 50% of people with eating disorders also abuse alcohol or drugs.
- This is a rate that is 5X higher than the general population.
- Similarly, 35% of substance abusers have an eating disorder.
- This is a rate that is 11X higher than the general population.
- Up to 70% of women in treatment for alcohol abuse have a history of binge-eating.
Specifically, in the case of Binge-Eating Disorders, 25% of sufferers also abuse substances.
Why Do Eating Disorders and Addictive Disorders Cooccur?
 There are several theories as to why addictive and eating disorders manifest together so frequently. The first theory is consistent with the findings that both excessive eating and excessive drinking activate the brain’s reward pathways. In other words, people surrender to the unhealthy urge, because it brings them an emotional reward. It makes them FEEL better, at least temporarily. The second theory is in response to the fact that many people who abuse alcohol or food are struggling with depression, anxiety, and/or some past traumatic event. They over-eat and over-drink as a way of “self-medicating”. Again, that reprieve is only temporary, because it only deepens their downward spiral. The third theory is based on recent research suggesting a genetic link between alcohol abuse and eating disorders. In 2013, Melissa-Munn Chernoff, a researcher with the Washington University School of Medicine, discovered that between 38% and 53% of the likelihood of developing either type of disorder is attributable to one set of genes. The fourth theory points to the discovery that both alcoholism and BED have been linked to poor impulse control. For example, women who have both conditions score higher on the impulsivity scale than women who only have one disorders.
There are several theories as to why addictive and eating disorders manifest together so frequently. The first theory is consistent with the findings that both excessive eating and excessive drinking activate the brain’s reward pathways. In other words, people surrender to the unhealthy urge, because it brings them an emotional reward. It makes them FEEL better, at least temporarily. The second theory is in response to the fact that many people who abuse alcohol or food are struggling with depression, anxiety, and/or some past traumatic event. They over-eat and over-drink as a way of “self-medicating”. Again, that reprieve is only temporary, because it only deepens their downward spiral. The third theory is based on recent research suggesting a genetic link between alcohol abuse and eating disorders. In 2013, Melissa-Munn Chernoff, a researcher with the Washington University School of Medicine, discovered that between 38% and 53% of the likelihood of developing either type of disorder is attributable to one set of genes. The fourth theory points to the discovery that both alcoholism and BED have been linked to poor impulse control. For example, women who have both conditions score higher on the impulsivity scale than women who only have one disorders.
What Do I Do If I Struggle with Both Binge-Drinking and Binge-Eating?
 Have both conditions means you have a dual diagnosis – an addictive disorder (to alcohol) occurring at the same time as a mental disorder (binge-eating). Either of these illnesses are hard enough to overcome on their own. But when they present together, the task becomes even more difficult. All treatment programs are not created equal. Many focus on one illness or the other, meaning they are not equipped or staffed to handle clients with a dual diagnosis. As a result, the untreated condition complicates – and even jeopardizes – your successful alcoholism recovery treatment. The safest way to get better is by finding a service provider that specializes in treating co-occurring disorders. Addressing both needs simultaneously makes treatment more individualized and effective, while at the same time reducing the risk of relapse from either.
Have both conditions means you have a dual diagnosis – an addictive disorder (to alcohol) occurring at the same time as a mental disorder (binge-eating). Either of these illnesses are hard enough to overcome on their own. But when they present together, the task becomes even more difficult. All treatment programs are not created equal. Many focus on one illness or the other, meaning they are not equipped or staffed to handle clients with a dual diagnosis. As a result, the untreated condition complicates – and even jeopardizes – your successful alcoholism recovery treatment. The safest way to get better is by finding a service provider that specializes in treating co-occurring disorders. Addressing both needs simultaneously makes treatment more individualized and effective, while at the same time reducing the risk of relapse from either.
Full Infographic:
Sources:
https://blogs.discovermagazine.com/d-brief/2017/01/10/binge-drinking-binge-eating/#.WS13Jo-cGsp https://www.nature.com/neuro/journal/v14/n3/full/nn.2739.html https://www.nature.com/articles/ncomms14014 https://www.sciencedirect.com/science/article/pii/S0195666315000306 https://onlinelibrary.wiley.com/doi/10.1002/oby.21109/full https://www.ibtimes.com/boozing-fatty-food-cravings-science-behind-hangover-brunch-1025394 https://ajcn.nutrition.org/content/62/3/639.abstract?ijkey=f2a27120ad2765a7ba324332e4c488762313eceb&keytype2=tf_ipsecsha https://www.sciencedirect.com/science/article/pii/S1555415510003120 https://www.researchgate.net/publication/23392554_The_Relationship_Between_Alcohol_Use_Eating_Habits_and_Weight_Change_in_College_Freshmen https://www.exercisemenu.com/does-drinking-alcohol-cause-overeating/#_ftnref https://www.sciencedirect.com/science/article/pii/S0031938401005984 https://www.nationaleatingdisorders.org/eating-disorders-substance-abuse https://www.usnews.com/news/articles/2013/08/21/same-genes-may-cause-alcohol-abuse-and-eating-disorders